Palliative Care EMR Tool: A case study on identifying patients that could benefit from a palliative approach to care
Key takeaway
The Palliative Care EMR tool provides decision support to primary care in identifying patients who could benefit from a palliative approach to care, supporting earlier patient identification and ensuring earlier management and treatment to improve patient outcomes.
Although 89% of Canadians nearing end of life could benefit from a palliative approach to care, only 15% actually received it.1 Timely access and early identification of those who could benefit from palliative care is associated with better patient and system outcomes.2-4 While primary care providers can play an important role in adequately meeting patients’ palliative care needs,5 only 37% are well prepared to manage patients in need of palliative care.6
Amplify Care (formerly the eHealth Centre of Excellence), in partnership with the Waterloo Wellington Integrated Hospice Palliative Care Regional Program, developed a palliative care electronic medical record (EMR) decision support tool, to assist primary care in early identification of patients who could benefit from a palliative approach to care. The EMR tool supports clinicians to assess their patients’ palliative care needs, conduct advance care planning, and engage in conversations with their substitute decision maker while also providing education to clinicians, patients, their families and caregivers.
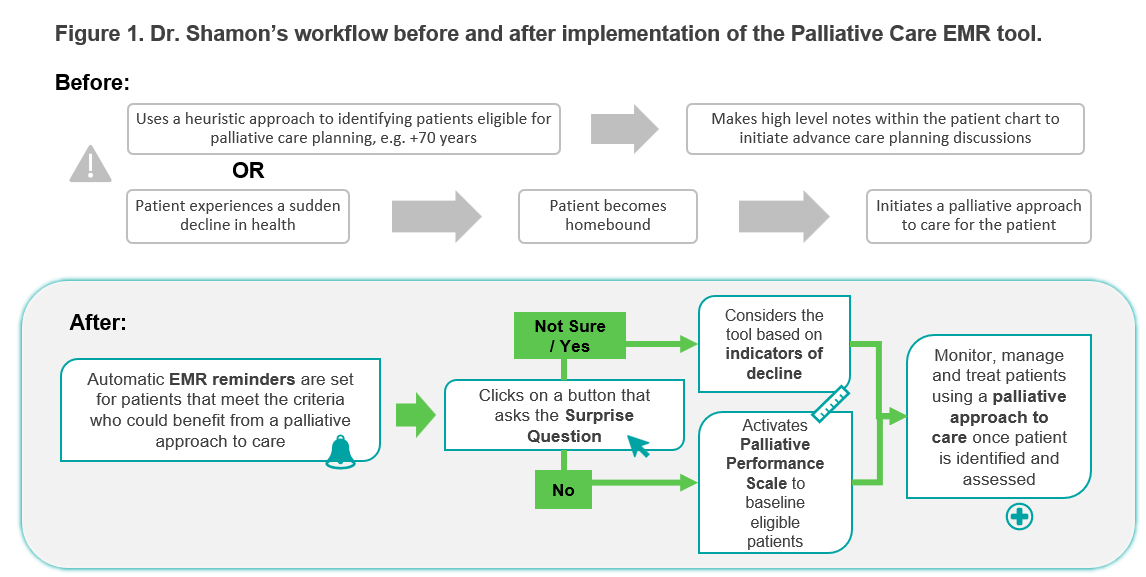
As a family physician, Dr. Sandy Shamon adopted the Palliative Care EMR tool in the Fall of 2019 to better facilitate a palliative approach to care within her primary care practice.
Using the EMR tool in primary care has helped me identify patients much earlier who would have otherwise been identified at a later stage. By gradually completing different components of the tool, I have standardized my documentation, enabling a palliative approach to care. For providers new to palliative care, I encourage them to start slowly; first record the patient’s [substitute decision maker] for a particular age group or chronic condition(s), and then build on other part of the form.
Dr. Sandy Shamom
Family Heritage FHO
Within five months of adopting the Palliative Care EMR Tool, Dr. Shamon has operationalized a standardized palliative approach to care within her primary care practice, identifying patients that would benefit from a palliative approach earlier. In the absence of the EMR tool, these patients would have otherwise been identified at a later time.
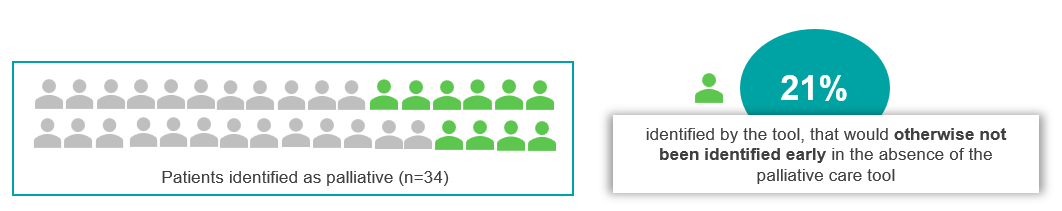
Dr. Shamon experienced the following benefits:
Early identification of patients
The tool highlights patients who may meet criteria
Early identification of palliative care needs has been associated with greater patient experience2 and reduced utilization of acute care services at the end of life4
Enable coordinated care for patients
Standardized notes on patient care goals can be readily shared with the patient’s transition team to support effective care planning, reducing the need for the patient to repeat their values and goals
Efficiently enable patient-centred care
Decision support provides the option of initiating conversations
with patients
The EMR tool captures patient values, wants and needs, ensuring care is centred on patient goals
Support billing practices
Palliative care services rendered in primary care are billed appropriately
Standardized notes are searchable and available for auditing purposes
For primary care clinicians who are not certain or would not have considered the patient for palliative care, the tool also provides guidance on what to consider based on “indicators of decline” as well as prompts for completing a baseline Palliative Performance Scale. The absence of a timely palliative approach to care may lead to providers being more reactive, focusing on efforts of managing patient expectations and working around the core health issue, rather than addressing the patient’s quality of life and mortality in support of whole-person care.
Works Cited:
- Canadian Institute for Health Information. (2018). Access to palliative care in Canada. Ottawa, ON:CIHI.
- Shippee, ND, et al. (2018). Effect of a Whole-Person Model of Care on Patient Experience in Patients With Complex Chronic Illness in Late Life. American Journal of Hospice & Palliative Medicine. 35(1):104-109.
- Hannon, B. et al. (2017). Experiences of patients and caregivers with early palliative care: A qualitative study. Palliat. Med. 31(1):72-81.
- Qureshi, D. et al. (2019). Early initiation of palliative care is associated with reduced late-life acute-hospital use: A population-based retrospective cohort study. Palliat Med. 33(2):150-159.
- Shadd, J.D. (2013). Defining and measuring a palliative approach in primary care. Can Fam Physician. 59(11):1149-1150.
- The Commonwealth Fund. (2019). The Commonwealth Fund 2019 International Health Policy Survey of Primary care Physicians.
Interested in learning more?
Interested in partnering with us or learning more about
what we can offer you? Please reach out here.
Get the latest resources and insights
-

Virtual Care: A case study on a midwifery perspective on video visits
In response to the increased cases of the novel coronavirus (COVID-19) disease, providers throughout the…
-

Fiscal year 22/23 eReferral highlights
eReferral deployment across Ontario, led by the Ontario eServices Program, contributed to a large degree…
-

How Grandview Medical Centre Reimagined the Clinic of the Future with CHIME
A look into how Grandview Medical Centre in Cambridge, Ontario, implemented CHIME, an AI-powered clinic-orchestration…
-

Virtual Care: A case study on virtual visits from a psychiatrist perspective
Virtual care enables psychiatrists to provide continuity of care to patients, enabling provision of specialized…